Hypopneas: Causes, Diagnosis & Treatment options
Published:
When it comes to sleep medicine, hypopneas are a crucial topic of discussion that often goes unnoticed. As a lesser-known aspect of sleep-disordered breathing, understanding hypopneas is essential for maintaining good health and achieving restful sleep.
Contents:
In this blog post, we will delve into the definition and characteristics of hypopneas, as well as the health risks associated with untreated cases. We'll also discuss the importance of accurate diagnostic tools in identifying respiratory events during sleep studies and how polysomnography-based algorithms can differentiate between central and obstructive hypopneas.
Furthermore, we will explore common causes leading to obstructive hypopneas and the role obesity plays in increasing one's risk for developing Obstructive Sleep Apnea (OSA). Additionally, you'll learn about normal ranges for hypopneas per hour and how their frequency impacts both sleep quality and overall health. Finally, we will examine various treatment options available for those struggling with sleep-disordered breathing issues such as lifestyle modifications or Continuous Positive Airway Pressure (CPAP) therapy.

Understanding Hypopneas
Hypopneas are partial blockages or reductions in airflow during sleep, often associated with obstructive sleep apnea (OSA). Accurate diagnosis is essential for recognizing both central and obstructive cases of this condition, as failure to do so can lead to serious health risks. Accurate diagnosis through polysomnography-based algorithms is crucial for identifying central and obstructive cases of this condition effectively.
Definition and Characteristics of Hypopneas
A hypopnea episode is when the air intake declines by at least 30% in comparison to a typical breathing pattern, together with either an oxygen saturation decrease or being woken up from sleep. These events typically last for at least 10 seconds but can vary depending on the individual's specific respiratory patterns. The severity of hypopneas may range from mild to severe, based on factors such as frequency per hour and impact on overall sleep quality.
Hypopneas differ from apneas, which involve complete cessation of airflow during sleep. While both conditions disrupt normal breathing patterns and contribute to poor sleep quality, they require different diagnostic criteria for accurate identification.
Health Risks Associated with Untreated Hypopneas
If left untreated, hypopneas can pose significant health risks due to their association with OSA. Some potential consequences include:
- Sleep fragmentation: Frequent arousals caused by reduced airflow result in disrupted sleeping patterns leading to daytime fatigue and impaired cognitive function.
- Oxygen desaturation: Reduced blood oxygen levels increase the risk of cardiovascular complications such as hypertension, heart failure, stroke, or arrhythmias.
- Metabolic disorders: Chronic sleep disruption has been linked to insulin resistance, type 2 diabetes, and obesity.
- Mental health issues: Poor sleep quality can contribute to mood disturbances like depression or anxiety.
To mitigate these risks, it is essential for individuals experiencing symptoms of hypopneas or OSA to seek proper medical evaluation and treatment. A thorough assessment by a qualified healthcare professional specializing in sleep medicine will help determine the most appropriate course of action based on individual needs and circumstances.
Sleep Studies and Hypopnea Diagnosis
Sleep studies remain the gold standard when it comes to diagnosing any kind of disorder related specifically towards disrupted patterns while unconscious. Polysomnography-based algorithms provide comprehensive insight into what might otherwise go unnoticed without proper examination from qualified professionals such as physicians specializing in sleep medicine.
The Importance of Accurate Diagnostic Tools for Identifying Respiratory Events
An accurate diagnosis is crucial for determining the most effective treatment plan for individuals with hypopneas or other respiratory events during sleep. Polysomnography (PSG) remains the preferred diagnostic tool due to its ability to monitor various physiological parameters simultaneously throughout an entire night's rest. This includes brain activity, eye movements, muscle tone, heart rate, blood oxygen levels, airflow through nasal passages or mouth opening (oronasal thermistor), chest wall movement indicating effortful breathing attempts (respiratory effort-related arousals), among other factors that may indicate abnormal respiration patterns associated with central or obstructive cases.

Sleep Studies and Hypopnea Diagnosis
When it comes to diagnosing sleep-related disorders, sleep studies are the gold standard. These tests provide invaluable insights into a person's sleeping patterns, allowing medical professionals to identify any disruptions that may be impacting their overall health. One such diagnostic tool is polysomnography-based algorithms, which play a crucial role in detecting respiratory events like hypopneas.
The Importance of Accurate Diagnostic Tools for Identifying Respiratory Events
Accurate diagnostic tools are essential for healthcare providers to identify sleep-disordered breathing issues such as obstructive sleep apnea (OSA). Polysomnography-based algorithms offer comprehensive data on an individual's airflow during sleep, enabling physicians specializing in sleep medicine to pinpoint specific respiratory events like hypopneas or apneas.
This level of detail allows doctors not only to determine whether someone suffers from OSA but also helps them differentiate between central and obstructive cases of the condition. By understanding the underlying cause of these respiratory disturbances, clinicians can develop more targeted treatment plans aimed at addressing each patient's unique needs.
How a Polysomnography-Based Algorithm Defines Central and Obstructive Cases
A polysomnography-based algorithm works by monitoring various physiological parameters throughout the night while an individual sleeps. Some common measurements include:
- Airflow through the nose and mouth using thermistors or nasal pressure transducers;
- Chest wall movement with thoracic impedance belts;
- Oxygen saturation levels via pulse oximetry;
- Brain activity through electroencephalography (EEG);
- EMG can be utilized to monitor muscular activity.
By analyzing this data, the algorithm can identify periods of reduced airflow or complete cessation of breathing. In the case of hypopneas, a partial blockage or reduction in airflow is detected. The algorithm then classifies these events as either central or obstructive based on additional information gathered during the sleep study.
Central hypopneas occur when there is a lack of respiratory effort due to issues with the brain's control over breathing muscles. This type of event typically presents itself alongside other neurological conditions and requires specialized treatment approaches. On the other hand, obstructive hypopneas are caused by physical obstructions within the airway that impede normal airflow despite ongoing respiratory effort from an individual.
In summary, polysomnography-based algorithms play a vital role in diagnosing sleep-disordered breathing issues like OSA and differentiating between central and obstructive cases. With accurate diagnostic tools at their disposal, healthcare providers can develop targeted treatment plans designed to address each patient's unique needs effectively.
Obstructive Hypopneas: Causes and Risk Factors
Obstructive hypopneas are partial blockages of the airway during sleep, which can lead to disrupted breathing patterns and reduced oxygen levels in the blood. To ensure early detection and effective treatment, it is important to understand the causes and risk factors associated with obstructive hypopneas. In this section, we will explore common causes leading to obstructive hypopneas, as well as how obesity plays a role in increasing one's risk for developing obstructive sleep apnea (OSA).
Common Causes Leading to Obstructive Hypopneas
The development of obstructive hypopneas may be attributed to various conditions that narrow or partially block the airway. Some common factors include:
- Anatomical abnormalities: Enlarged tonsils or adenoids, deviated nasal septum, or other structural issues within the upper respiratory tract can contribute to airway obstruction.
- Muscle relaxation: During sleep, muscles in your throat relax more than usual due to decreased muscle tone. This relaxation may cause narrowing of your airways.
- Inflammation: Allergies or infections causing inflammation in your nose and throat might also result in a narrowed air passage.
- Lifestyle factors: Alcohol consumption before bedtime has been shown to increase muscle relaxation and decrease overall muscle tone throughout nocturnal hours each night on a regular basis.
The Role of Obesity in Increasing Risk for Developing OSA
A major contributing factor towards an increased prevalence of hypopnea-predominant OSA is obesity. Excess body weight, particularly around the neck and chest areas, can lead to increased pressure on the airway and a higher likelihood of obstruction during sleep. According to the American Academy of Sleep Medicine, obese individuals are at least four times more likely to develop OSA compared to those with normal body weight.
Furthermore, research has shown that women seem more susceptible than men when it comes to developing hypopneas due in part because they tend towards carrying excess fat in their upper bodies rather than lower regions like hips or thighs as males typically do (source). This difference may result in greater constriction within female airways leading up towards instances where partial blockages occur throughout nocturnal hours each night on a regular basis.
In addition to obesity, other risk factors for obstructive hypopneas include:
- Age: The prevalence of OSA increases with age, especially among middle-aged adults and older individuals.
- Family history: Having family members who suffer from sleep apnea might increase your chances of developing this condition yourself.
- Gastroesophageal reflux disease (GERD): People suffering from GERD often experience acid reflux while sleeping which can cause inflammation and narrowing of the throat passages contributing further towards development or worsening symptoms associated specifically toward disrupted patterns while unconscious such as snoring or choking throughout nocturnal hours each night on a regular basis (source).
Grasping the source and potential dangers of obstructed hypopneas is essential for early discovery, identification, and management. By addressing these underlying issues through lifestyle modifications or medical interventions, individuals can significantly improve their sleep quality and overall health.
Normal Ranges & Frequency of Hypopneas per Hour
Identifying how many hypopneas per hour is normal plays a significant role in determining whether someone suffers from a sleep-related breathing disorder like obstructive hypopneas. It's important not only for patients but also for their partners who may experience disturbances due to symptoms like snoring and choking throughout nocturnal hours each night on a regular basis.
Defining Normal Ranges for Hypopneas per Hour
The number of hypopneas considered normal varies depending on the individual and their specific circumstances. Medical professionals typically use the Apnea-Hypopnea Index (AHI) as a benchmark for evaluating sleep apnea severity, which calculates the average number of apneas and hypopneas occurring per hour during sleep. The AHI calculates the average number of apneas and hypopneas occurring per hour during sleep. According to the American Academy of Sleep Medicine, an AHI score can be categorized into four levels:
- Normal: An AHI less than 5 events per hour is considered within normal limits.
- Mild Sleep Apnea: An AHI between 5-15 events per hour indicates mild sleep apnea.
- Moderate Sleep Apnea: An AHI between 15-30 events per hour suggests moderate sleep apnea.
- Severe Sleep Apnea: An AHI greater than or equal to 30 events per hour points towards severe sleep apnea.
If you suspect that you or your partner might have abnormal rates of hypopneas, it's crucial to consult with a healthcare professional specializing in sleep medicine for proper evaluation and diagnosis.
The Impact of Frequency on Sleep Quality and Overall Health
Experiencing frequent hypopneas can have a significant impact on sleep quality, leading to poor overall health. When the airway is partially blocked during sleep, it may cause oxygen levels in the blood to drop. This decrease in oxygen triggers the brain to awaken briefly and restore normal breathing patterns, disrupting restorative sleep.
Poor sleep quality due to hypopneas can result in various short-term and long-term consequences. Some immediate effects include excessive daytime fatigue, irritability, difficulty concentrating, or memory problems. Over time, untreated apneas and hypopneas may contribute to more severe health issues such as high blood pressure (source), heart disease (source), type 2 diabetes (source), stroke (source) or even depression.
To maintain optimal health and well-being, it's essential for individuals experiencing abnormal rates of hypopneas per hour to seek professional help from a qualified healthcare provider specializing in sleep medicine. Early intervention through accurate diagnosis and appropriate treatment options can significantly improve one's overall quality of life by addressing these underlying respiratory events that disrupt healthy sleeping patterns.
Treatment Options For Sleep-Disordered Breathing Issues
Dealing with sleep-disordered breathing issues such as apneas and hypopneas can significantly impact an individual's quality of life. Fortunately, there are various treatment options available that aim to alleviate the symptoms associated with these conditions, reduce their frequency or severity, and ultimately improve overall health outcomes for patients suffering from them.
Lifestyle Modifications to Address OSA-related Symptoms
Making certain lifestyle changes can be a helpful first step in managing obstructive sleep apnea (OSA) and related symptoms like hypopneas. Some recommended modifications include:
- Weight loss: Since obesity is a significant risk factor for developing OSA, losing weight may help reduce the occurrence of apneas and hypopneas.
- Avoiding alcohol and sedatives: These substances can relax the muscles in your throat, increasing the likelihood of airway obstruction during sleep.
- Sleep position adjustments: Sleeping on your side instead of your back may help keep your airway open by preventing gravity from causing your tongue to fall back into your throat.
- Nasal decongestants or allergy medications: If nasal congestion contributes to breathing difficulties during sleep, using over-the-counter decongestants or prescribed allergy medications might provide relief.
CPAP Therapy as an Effective Treatment Option
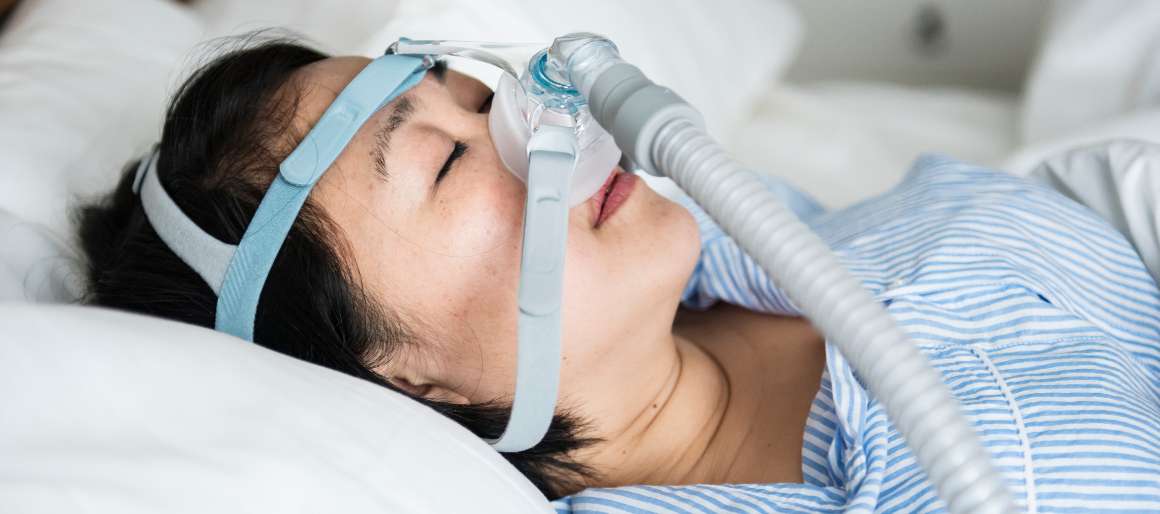
The most common treatment option for moderate-to-severe cases of OSA is continuous positive airway pressure (CPAP) therapy. This involves wearing a mask connected to a machine that delivers pressurized air through the nose or mouth, keeping the airway open and preventing apneas and hypopneas from occurring.
CPAP therapy has been proven to be highly effective in reducing sleep-disordered breathing events. However, some patients may find it challenging to adapt to wearing a mask during sleep. In such cases, alternative treatment options include:
- Bilevel positive airway pressure (BiPAP): Similar to CPAP but provides different levels of pressure for inhalation and exhalation, making it more comfortable for some users.
- Adaptive servo-ventilation (ASV): A newer form of positive airway pressure therapy that adjusts airflow based on an individual's breathing patterns.
In addition to these treatments, other interventions like oral appliances or surgery might be considered depending on the severity of OSA and specific patient needs. Oral appliances work by repositioning the jaw forward during sleep, opening up the airway space at the back of your throat. Surgical options can range from minimally invasive procedures like radiofrequency ablation (RFA) that shrink tissue causing obstruction in your throat to more extensive surgeries such as uvulopalatopharyngoplasty (UPPP) which removes excess tissue from your soft palate and pharynx area.
Treating sleep-disordered breathing issues is crucial not only for improving nighttime symptoms but also for addressing potential long-term health risks associated with untreated conditions like OSA. Consult with a healthcare professional specializing in sleep medicine, such as the American Academy of Sleep Medicine, to determine the most appropriate treatment plan for your specific needs.
FAQs in Relation to Hypopneas
What is the 4% rule for hypopnea?
The 4% rule for hypopnea refers to a diagnostic criterion used in sleep studies, where a hypopneic event is considered significant if it results in at least a 4% drop in blood oxygen saturation. This helps differentiate between normal fluctuations and clinically relevant respiratory events that may require treatment.
Are hypopneas as bad as apneas?
Hypopneas are generally less severe than apneas but can still have negative health effects if left untreated. Both conditions disrupt normal breathing patterns during sleep, leading to fragmented sleep and reduced overall sleep quality. However, apneas involve complete airway obstruction while hypopneas only involve partial obstruction or reduction of airflow.
What is the 3% hypopnea rule?
The 3% hypopnea rule refers to an alternative diagnostic criterion where a decrease of at least 30% in airflow lasting for more than ten seconds accompanied by at least a 3% drop in blood oxygen saturation defines a significant hypopneic event. This threshold allows clinicians to identify milder cases that may still impact overall health and well-being.
What are the long term effects of hypopnea?
If left untreated, chronic occurrences of hypopnea can lead to various long-term health issues such as excessive daytime fatigue, impaired cognitive function, mood disturbances like depression or anxiety, cardiovascular problems including hypertension and arrhythmias, metabolic disorders like diabetes mellitus type II or insulin resistance syndrome among others.








